A group of medical staff from Gwent has transformed the lives of people living in a part of Ethiopia. Argus digital editor MARTIN WADE, pictured, travelled with them to the African country to see their work first-hand.
THE young Ethiopian pair were clutching each other and dancing awkwardly. This in itself wasn’t that unusual in Ethiopia, where the sound of dance music is never far away. What made this remarkable was that we were in a hospital and they were dancing because a midwife from Gwent was telling them to do so.
The dancing was to get midwifery students to see how a woman in labour could feel comfortable by clutching a partner and almost waltzing across the floor.
When you say “Ethiopia” to people in the UK, the image many people will have is of starving children in flyinfested refugee camps.
In southern Ethiopia when I visited with a group of Gwent health workers, there were no people dying of hunger. But the risks to health were still stark.
The country has an appalling rate of maternal death, with 561 women dying for every 100,000 live births.
As well as that, if a mother dies in childbirth in Ethiopia, the rest of her children generally will die within a year.
I travelled to the nation earlier this month with the Gwent-Southern Ethiopia Link. Set up 12 years ago to give training and equipment to health workers in the region, it was founded by Nevill Hall consultant surgeon Biku Ghosh in Gwent and Dr Aberra Gobeze in Ethiopia.
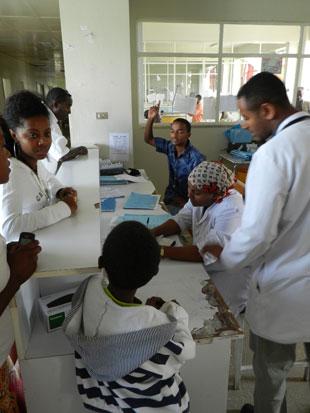
The lesson with the midwives was one of many given in the southern regional capital, Hawassa. Its university hospital is a similar size to Nevill Hall in Abergavenny. While it sits in the green foothills of the Black Mountains with traffic trundling by on the A40, the road to Hawassa hospital is lined with shops made of tin sheet or mud and daubed with bright colours. Drivers must weave between donkey carts, cyclists and wandering livestock.
Much of the teaching is hands-on.
There is the dancing of course, and some of the sessions use a model pelvis and doll to show possible problems in childbirth. The Welsh midwives even put on a play to show bad and good practice. They instruct trainers who then go out to regional centres to teach midwives.
The training is clearly valued.
One student, Firew Tirwheh has travelled for four days to cover 800km to be at this course.
“I’ve come here to skill up” he says proudly, “this will help us to reduce maternal mortality.”
It is not just training the Link will give here.
Doctors join their Ethiopian colleagues on the wards, giving advice and guidance.
On one such tour, Nevill Hall paediatrician Dr Peter Dale made a shocking discovery.
He found an ex-Royal Gwent incubator donated by them two years ago. It sat unused, seemingly broken, in a back room.
As the incubator was not working, three premature babies lay loosely swaddled on a bed next to an electric radiator, on full and leaning precariously.
Peter tells me how vulnerable premature babies are: “They can’t keep themselves warm. If they’re left in the open they will cool down too much as they have very little body fat.”
The incubator is a simple and robust type, he says and if he can fix it, those premature babies might stand a better chance. With a new plug fitted and wiring checked, the machine blinks into life.
Much equipment is given to developing countries, and much goes wrong and can sit rusting. Because the Link returns every six months they can look in and see if things are still working.
Elsewhere in the hospital, Nevill Hall gynaecologist Essam el-Hamamy taught students and GPs from smaller regional hospitals about difficult challenges like a restricted umbilical cord and emergency Caesarean section.
Yassir Younis is a second year emergency surgery Masters student.
“The training was very interesting and very useful. I liked the practical part and the group discussions. I am honoured to be here.” Royal Gwent consultant Dr Jill Curtis too feels privileged to be here: “It teaches you humility” she says.
Dr Curtis is teaching anaesthestists with Welsh colleagues.
Much of their teaching covers maternal health, with the students looking at how to deal with life-threatening conditions women in labour are at risk from.
Yasu Albaina, an anaethstist at Hawassa hospital, says he is learning valuable new skills: “We are learning to put drips in people – these new skills help make us better at our jobs.”
A key part of all training given by the Link is the teaching of teamwork – that all health workers have a part to play in delivering babies safely and keeping mothers healthy.
A message given again and again is that they should not be afraid to ask for help.
It’s the same urge that made Mr Ghosh and Dr Gobeze set up the Link. The very human desire to help. Equally, many of the Gwent workers enthuse about what they get back from the visits.
“You can practise real medicine here.” Dr Peter Dale tells me.
“While in the UK, you’re not always directly saving people’s lives, here you often are.”
Dr Curtis agrees: “We bring a lot of lessons back about making do and getting by without huge resources.”
Mr Ghosh is clear about what they give and why.
“In a country of 83 million there are only 3,000 doctors and 85 per cent of people live in rural areas hundreds of kilometres from the nearest hospital. The only healthcare that these people can get is in rural health centres.
“It is here that we can help keep mothers and babies healthy.”
It is then a story of committed people from Gwent and Ethiopia working to pass on their knowledge, experience and even their dancing skills to help improve people’s lives in a place far away. It is a story of ordinary people doing extraordinary things.
● Tomorrow, MARTIN WADE takes a look at the work of the Gwent staff in rural health centres in Ethiopia’s deep south.






Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules hereComments are closed on this article